75+ Feeding Therapy Tips & Strategies
Posted by Debra C. Lowsky, MS, CCC-SLP on 15th Jun 2016
For any therapist seeking to specialize in feeding, the best piece of advice I could give you is to become a sponge. Take courses and workshops, read as many articles as you can, talk to and learn from your colleagues, join special interest groups on Facebook and ASHA etc., follow blogs, observe other therapy sessions, and don’t forget - learn from the children you treat as well. They will be your best teachers.
Feeding issues are complex. So take in as much information as you can from as many outlets as you can. But, take it all in with a grain of salt, because not every strategy will work for every child. Over the past 35 plus years, a number of people have told me that their way was the only way. Although that certainly would have made my job easier if it were true, I’ve never been able to use any one method “by the book.” Each child is different, so it will be up to you to evaluate their needs and cater treatment accordingly.
.

.
A long time ago my father-in-law gave me a piece of advice that has stuck with me ever since - listen to what everyone suggests, consider it graciously, and then do what’s right for you. In therapy, this means learning all of the different techniques out there, having all of it in your “bag of tricks” as resources, and then deciding which strategies are appropriate in which situations.
To any parents who may be reading this: if you're concerned about your child’s feeding development or any eating problems, I cannot stress enough the importance of finding an experienced feeding therapist to do an evaluation. No article online or otherwise is an adequate substitute for an in-person evaluation with a trained professional. We don’t bite - trust me! But we will do our best to help your child take a bite.
Below are some pediatric feeding therapy techniques that have been effective with the children I have personally seen for feeding therapy. It is my sincere hope that some of these feeding therapy activities are helpful for you as well:
.
GENERAL:
• Be an investigator. Any underlying medical reasons for refusing foods must be managed first, so discuss with the pediatrician, study the medical history, and refer out for additional tests/evaluations when necessary. Are there any GI issues for instance? Reflux? If so, those must be handled first. I don’t recommend any oral intervention until all medical issues have been handled, as that can create more aversions. Don’t forget seeing a dentist to rule out any underlying issues there, too.
• Consult with other professionals: a nutritionist, a physical therapist for positioning, an occupational therapist for sensory, etc. Treating individuals with feeding problems requires a team approach.
• Try to get to the root of why they are refusing foods and work from there. Is it oral motor and/or sensory related? Is it oral defensiveness? Texture aversions? Perhaps they didn't go through a mouthing phase? Etc.
• Establish trust first. Assess the situation - if the child seems hesitant or not fully at ease with you in the first session, just talk and play games and be goofy. It's important that the child feels comfortable with you before starting any feeding intervention. This may take a few sessions or even longer to establish rapport.
• Be calm and supportive. Children can be very adept at sensing any frustration, overeagerness, being in a rush, etc. so constantly monitor what emotions you are displaying. Work at maintaining a stress-free therapy atmosphere by staying relaxed, patient, and showing them that you care.
• Never force a child to mouth, bite, chew, lick, or taste anything. I can't emphasize this enough.
• Be flexible and willing to adapt on a whim. If the child is showing interest in a particular doll - Great! Use that doll in therapy. Feed the doll. Have the doll feed you. Have the doll feed the child. What kinds of foods does the doll like? And so forth. The same goes for speech therapy as well. Use the child’s interest(s) to your advantage to get the best results.
• Get the parents involved - they must follow through at home.
• Get anyone else who has direct contact with the child (aunts, siblings, grandparents, friends, early interventionists, etc.) on board as well. The best results happen when therapy is reinforced at home in between sessions. The more opportunities presented, the better.
• Keep in mind that food refusals are often because of a very real fear. Respect this fear and support them through it.
• Follow the child's lead. If he likes potato chips - great! We can work from there. If he's showing signs of grimacing, pushing away, turning his head away, etc., stop and move on to something else. It's important to stop BEFORE the individual gets overloaded.
.
.
BEFORE FEEDING:
• Establish a routine. At the beginning of feeding therapy, my kids know to come in and wash their hands first. I have a visual schedule in the kitchen showing them to turn on the faucet, get some soap, wash their hands, get a paper towel, dry their hands, throw it away, and then come to the table. This routine lets them know what to expect and gives them confidence in that, alleviating some of the "fear of the unknown." It also works on following directions, sequencing, and independence.
• Make sure the child understands the vocabulary involved - bite, chew, etc. Demonstrate how to bite so that the child can see and learn what the word actually means. Knowing the vocabulary will be an important part of therapy as you encourage the child to bite and chew. Over-exaggerate the movement to help teach the concept.
• Start by talking about and exploring pretend food first if necessary.
• Get the child involved in the kitchen. If they have a hand in preparing the food (even if it’s a small task like bringing their bowl from the kitchen to the table), they may be more willing to try it. And even if they don’t end up trying it, interacting with the food is still a positive step.
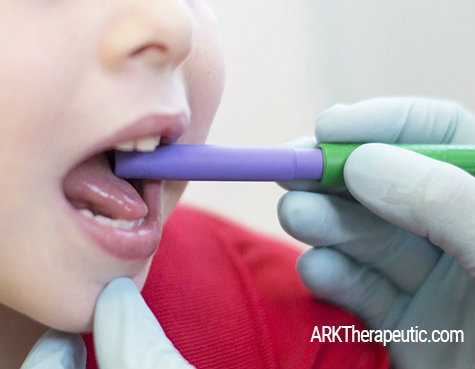
• Do sensory stimulating activities before feeding, such as sensory play, exploring a tactile wall, stimulating the lips, tongue, and cheeks with the Z-Vibe, etc.
• Encourage chewing on / mouthing a Textured Grabber and/or Y-Chew. Especially if a child didn’t go through a normal mouthing phase, this helps introduce them to new textures and sensations, allows them to safely explore the pockets and shapes with their mouth and tongue, increases sensory awareness, provides tactile input, etc. Try dipping these in puréed foods later on.
• If there are any sensitivities throughout the body, these will typically need to be addressed first before you can fully normalize sensitivities in the mouth. This is one area where an occupational therapist can really help. They may recommend things like swinging or jumping before therapy, weighted blankets, sensory play, vibration, etc. to regulate the sensory system. Once it’s regulated, the child will usually be more open to exploring new foods.
.

.
PRESENTATION
• Use cookie cutters to cut food into different fun shapes. Have the child help you.
• Use divided plates for kids who don’t like their foods to touch. Try putting a new food in one of the sections. They don’t have to try it - it’s progress even if they just allow it to be there.
• Give foods playful names, like "banana boats" or "pretzel light sabers.”
• Taste the food yourself to make sure it actually tastes good.
• Offer lots of dipping options. Take what they like and try dipping it into something new. Can just be a TINY bit.
• Use spoons that are fairly shallow and easy to remove food from. They should also be smaller rather than bigger so that the spoon is not overloaded with giant sized bites - it’s a spoon not a shovel :). Our Spoon Tip was designed with this in mind.
• Use proper spoon feeding technique.
• For any tools/utensils you use, talk about them and let children feel and explore them first.
• Use clear or translucent cups/bottles so that they can see what’s in it before they take a sip, which may help reduce stress.
• If a child won't eat with a spoon, use whatever he/she WILL accept. Their fingers, a Grabber, Z-Vibe, Animal Tip, carrot, twizzler, etc. Sometimes something other than a traditional spoon/fork is less threatening.
• If a child won’t eat from a bowl, try putting it in a cup OR right on the high chair / clean table. Mix it up.
.

.
FEEDING:
• Make sure the feet are stabilized solidly on the ground with the back flat against the back of the chair. Consult with a PT on positioning if necessary.
• Use what they already like as a bridge to transition to new foods. If the child likes applesauce, put a little applesauce on a cracker. They might just try that too, or at least lick it off.
• Try making very small changes to foods that they already accept. Do they like carrots? Try steaming them slightly or presenting them differently. Do they like crackers? Try putting a TINY bit of a mild condiment on it. Try a different brand of the same food, or a different shape. Add a tiny bit of a certain spice. And so forth. People in general don’t like change, and kids are no exception, so keep the changes very small.
• Give them control where possible by letting them make choices. Let them choose which spoon they want, if they want juice or water, if they'd like to kiss the apple 3 times or lick it once, etc. Two choices are usually best - enough for them to have options without be overwhelmed by them.
• Throughout the intervention, make sure that you're telling the child what you’re doing and why. Knowing what's coming can be very helpful in reducing anxiety.
• Try new foods at snack time instead of mealtimes, so there is less pressure to get mealtime calories in.
• Model by eating the foods yourself (kids often learn through imitating). You can also model on a puppet or stuffed animal.
• Take breaks between bites. Swallow, count to three, take a sip of water, bite again.
• Let them feed you and/or mom, grandma, etc.
• Chew the food yourself to see how many chews are required. Then count it out loud with the child as he/she chews, or chew to a beat / song. This can help set a pace if they’re eating too fast. Ideally you want a rhythmic chewing pattern. It can also help make sure they’re fully chewing the food.
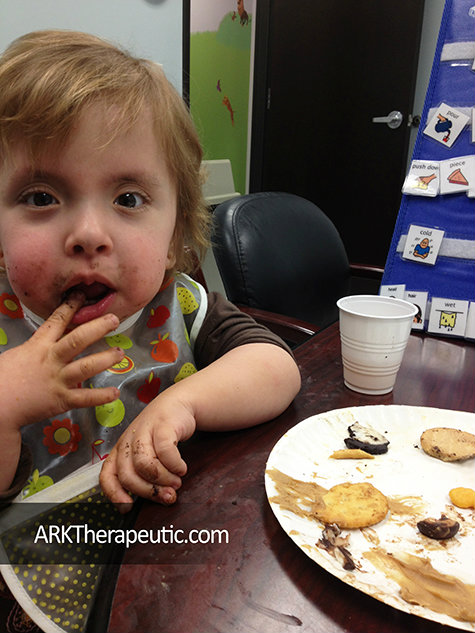
• Don’t be afraid to make a mess. I have parents who bring a change of clothes for after feeding therapy :)
.
.
• Encourage the parents to resist cleaning up, wiping off the child’s face/hands, etc. until the end of the meal.
• Take the pressure completely off. Let the child know that if they don’t like something, it’s ok to spit it out.
• If the child doesn’t want to try something, that’s ok. Let them know they can put it in the “no” bowl to be done with it - they may just touch it if it’s to move it off their plate.
• Teach the child how to do a lingual sweep to remove food from their mouth, with their tongue and/or with their finger if they can’t do it with their tongue yet. If the child has an "exit strategy" on how to remove food from their mouth, they’ll likely feel safer giving new foods a try.
• Try telling the child NOT to eat something (reverse psychology). I once said to a child, “would you like to give that graham cracker a kiss? Don’t eat it, just a quick kiss.” And lo and behold, she tried it. I said with animation, “Oh you're not supposed to eat it! You're supposed to just kiss it!” Ohhh she giggled and thought it was hilarious. Now I know that to get her to try something, I tell her not to try it. For most of my kids it's just about finding what makes them tick / what motivates them.
• When it comes to food aversions, children first need to become comfortable with food, which is usually a gradual process. What I do is introduce foods through play - I put food in front of the child and let them explore it with their hands - they can smash it, squeeze it, swirl it on the table, paint with it, etc. You may need to demonstrate and get involved in the play. It will get messy, and that's ok! The child may end up eating or tasting the food, which would be great, but the main goal is to get them playing with food, experiencing new sensations, and feeling more comfortable and safe around food.
• Use the element of surprise. I have literally taken a container of yogurt before and plopped the entire tub upside down onto the table (see the picture below). The child was so surprised 1. that I did that and 2. that she could play with it, that she ended up tasting food for the first time that day. It turned her usual associations with / expectations of food upside down (literally), which in turn made her more open to exploring it.
.

.
• Play with food without any pressure to actually eat it. Let them learn about it in a fun, comfortable, non-threatening way. Talk about it, using all 5 senses to describe it. See if they will touch it, blow on it, or kiss it. If they don’t want to, that’s ok. See if they will play with it with their fork, or maybe even use a carrot or another type of food to touch it instead (which would still be a win). And so forth.
• Try having the child blow food across the table - any kind of interaction with the food can be progress. See if they’ll blow it across the table with a veggie stick or one of those twizzlers with a hole in the middle.
• Very averse children may not even be able to tolerate being in the same room as a certain food. Gradually, over time and with other interventions, you can start moving the food just inside the door, then to the table, then to their plate, etc. Eventually they may touch it or even lick it, then they may hold it in their mouth for a moment before spitting it out. Eventually they will be comfortable enough to chew and maybe swallow it. Take your time, and allow the child to take their time. This process may take a looong time and that’s ok - don’t rush.
• For oral defensiveness, do gum massage before mealtimes and throughout the day. Work on normalizing sensation.
• Try providing oral input with the Z-Vibe. It has a smooth gentle vibration that can help “wake up” the mouth. Sometimes kids simply need a little extra input to know where there lips are, to feel the food, etc. Vibration can also help de-sensitize orally averse children.
• For low oral awareness, use a mirror and let kids watch themselves eating. This may help them better see and be more aware of what’s happening. Put some peanut butter, yogurt, pudding, etc. in their cheeks and have them fish it out with their tongue (this is great oral motor practice, too). Make it a game! Have the parents change up the type of toothbrush, toothpaste, and how the child brushes as well. For instance, if they always starts on the right side, have them start on the left side. The goal is to “mix things up” orally to increase awareness.
• Place the Probe, chew tool, Z-Vibe tip, etc. in the freezer to make it cold. The cold can help increase awareness / focus.
• Use the Probe, Grabber, and/or Y-Chew as “dipper spoons” for purées. This helps to introduce new textures and to practice biting/chewing in preparation for more advanced foods.
.

.
• Be careful what you put in front of children with oral motor delays, as they may not be able to orally manage certain foods yet. Try the foods yourself to make sure they are at the right level. Work on rotary chewing.
• Assess the child’s oral motor skills. If the child is functioning at an 8-month-old age level, for example, go back to the skills that a child should have at that age and build from there. The main oral motor skill to watch out for when it comes to manipulating food is tongue lateralization. The child will also need lip closure, jaw strength, jaw grading, tongue tip elevation, back of tongue elevation, tongue bowl, etc.
• When feeding, try to position the food to the sides of the mouth and/or in the cheeks (not always on the middle of the tongue). The goal of this is to encourage the tongue to move from side to side to develop tongue movement and lateralization.
• Be creative. Or as I like to say in relation to feeding therapy, "think outside the plate." Make a marshmallow snow man. Play tic tac toe with pieces of food as the "players." Make up a story and have pretzel people jump into a pool of yogurt and swim laps. And so forth. The sky is the limit.
.
MORE:
• Skip sippy cups - go straight to straw drinking for the most oral motor benefit, ideally with a Lip Blok.
• When teaching cup drinking, if thin liquids are too difficult for the child to manage, try thickening it with puréed baby foods or try letting them drink a tiny bit of the puréed food from a cup.
• Have the parents keep a food diary, documenting everything the child eats and drinks for 3-5 days. Have them note quantities AND any problems so that you can have more background.
• Take a look at preferences of family members - if mom doesn't like xyz, the kids might not either. Personally, I hate coffee and mushrooms, and guess what - so do my own kids. Some food preferences can be environmental.
• Individuals being fed via tube may still have the urge to bite/chew. Provide stimulation to the tongue, lips, cheeks, and gums with the Probe or Z-Vibe as if they were eating while being fed via g-tube. Let them chew on a Grabber or Y-Chew during tube feedings.
• Keep the environment calm and relaxed. For some children, that may mean sitting on the floor instead, or at a desk or craft table (perhaps child-sized), in another room of the house, outside, etc. The kitchen may be too stigmatized, so getting them out of that setting may help. It may also help to keep environmental distractions (other stuff in the room) to a minimum.
.

.
• Try using a mirror for visual feedback. Just keep in mind that for some children, this may be too distracting.
• A note on reflux – I have known parents to take their children off their medication without consulting the pediatrician. They usually do this between the age of 2 and 3 years because their child appears to be symptom-free. But then feeding issues begin or begin again. So, please remind parents to consult with their pediatrician first before doing so.
• If the child doesn’t like a food after the first presentation, keep trying. It may take 8-10 exposures or more before the child will be willing to try it.
• Keep in mind that it's completely normal to not like certain foods. I can't eat mushrooms because the texture is too slimy/spongy for me. The smell of coffee gives me a headache. And I stay away from powdered sugar because I tend to inhale it as I eat, which causes me to cough. All of this is 100% okay. I dare you to find someone who likes every food out there! So if you can't get a child to eat say pumpkin - that's ok. The goal is not to become an omnivore. The goal is to expand the diet to the point where the child can eat a healthy variety of foods.
• Remember to praise, praise, praise. Use reinforcements that cater to the child’s interests. Get excited about every milestone, no matter how small it may seem.
• Count on curveballs. It may not be a straight path, but you will get there.
Helping a child through feeding problems can be a long process. It's a marathon - not a sprint. So hang in there! Each child is different; there is no “one way” to do feeding therapy. What works for one child, may not work for the next, so this list is by no means all-inclusive or relevant for everyone. Kids don’t come with instructions, so be prepared for trial and error, and trying again. Play detective to get to the root of the problem. Trust your instincts. Listen to the parents. Listen to the child and follow their lead. Be creative. And don't forget to have fun!
.
Happy feeding,
Debbie
Debra C. Lowsky, MS, CCC-SLP
.

